The Untapped Potential of a Simple Shot
Every year, a heartbreaking ~ 342,000 women lose their lives to cervical cancer worldwide. Even more alarming is the fact that a staggering 80% of cases and 90% of deaths occur in low-and middle-income countries (LMICs).
It’s disheartening to consider that many of these women could have been safeguarded from the most prevalent cause of cervical cancer—the human papillomavirus (HPV)—through a safe and effective vaccine. Global immunization data released earlier this week brings optimism, indicating that HPV vaccination has surpassed pre-pandemic levels with mean coverages reaching 55% for LMICs, but still falling below the 90% global target. In LMICs, where access to alternative prevention methods like HPV screening and treatment is limited, HPV vaccination becomes increasingly important.
Why, then, is the uptake of the HPV vaccine still low in LMICs?
Since its introduction in 2006, the HPV vaccine has revolutionized the approach to preventing cervical cancer, becoming a cornerstone of prevention efforts. In 2012, Gavi, the Vaccine Alliance, took a commendable step by gradually introducing the HPV vaccine in select LMICs. However, despite these efforts, the reach of vaccination remains limited to only 29 countries, targeting adolescent girls aged 9-14 years through school-based platforms to improve programmatic coverage and efficiency.
To compound the issue, the integration of the HPV vaccine into routine immunization programs is still limited to approximately 125 countries (64%)—primarily those with higher incomes. Many LMICs that have implemented HPV vaccination programs face various challenges, such as vaccine procurement, supply chain logistics, securing favorable pricing agreements, and overall vaccine costs. These challenges further burden LMICs, which already struggle with efficient delivery and monitoring of vaccinations.
However, amidst these challenges, there are 4 clear opportunities to help overcome the barriers associated with HPV vaccination coverage in LMICs:
- LMICs should embrace a single-dose strategy for HPV vaccination: This transformative approach offers numerous advantages, including extended availability of vaccine supplies, reduced costs, and simplified distribution processes, alleviating the burden on health care budgets and making HPV vaccination more feasible and sustainable.
- LMICs need to play an active role in shaping sustainable markets, funding mechanisms, and policies that incentivize the integration of HPV vaccines into routine immunization programs and reduce existing inequalities. An ideal market scenario would involve multiple manufacturers offering HPV vaccines—creating a thriving environment that promotes innovation, recognizes inventive contributions, and reinforces the excellence of the HPV vaccine among payers and governments alike.
- Diversify delivery channels beyond school-based platforms: Reaching a broader population of adolescents, including those who are not enrolled in formal education or face barriers to regular school attendance, is critical to ensure that every adolescent girl—regardless of her educational status or access to school-based facilities—has an equal chance of receiving the HPV vaccine.
- Build community acceptance and trust: Community health workers can foster trust, dispel rumors, and promote vaccine uptake by establishing transparent and open lines of communication and addressing doubts and misconceptions about HPV vaccines. For instance, Tanzania actively engaged with community and religious leaders, and media personnel, through sensitization and awareness campaigns. When misinformation surfaced, health communication specialists effectively communicated accurate information via radio channels. Collaborating with community health workers and local stakeholders helps identify and overcome vaccination barriers, develop customized strategies, and implement culturally sensitive communication approaches.
We must recognize the toll of cervical cancer deaths is highly preventable. Each loss of life is a poignant reminder of the urgency and importance of the global mission to scale HPV vaccination. We can and must regain lost ground and move forward to a world where cervical cancer is no longer a threat to the lives of women.
Ahmed Haji Said MBBS, MPH is a doctoral student in the Global Health and Development program at Emory University, Rollins School of Public Health. He is a mixed-methods researcher with interests in vaccine equity, high-impact and sustainable solutions for vaccination programs, and social and behavioral factors that can influence public trust in vaccines.
Join the 50,000+ subscribers in 170+ countries who rely on Global Health NOW summaries and exclusive articles for the latest public health news. Sign up for our free weekday newsletter, and please share the link with friends and colleagues.
https://www.globalhealthnow.org/subscribe
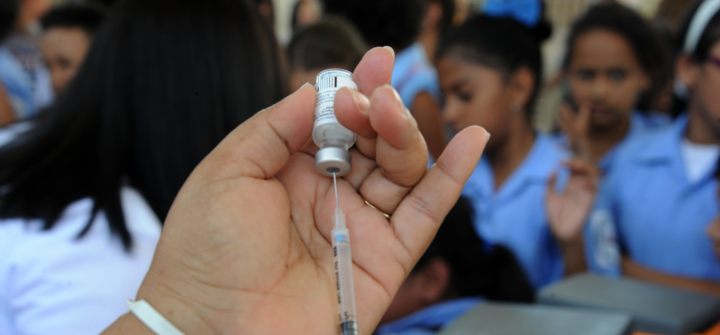
A health ministry employee prepares to vaccinate girls against the human papilloma virus in Tegucigalpa, Honduras, on May 17, 2016. Image: Orlando Sierra/AFP/Getty