Fighting the ‘Million-Murdering’ Mosquito: Lessons from the Pandemic
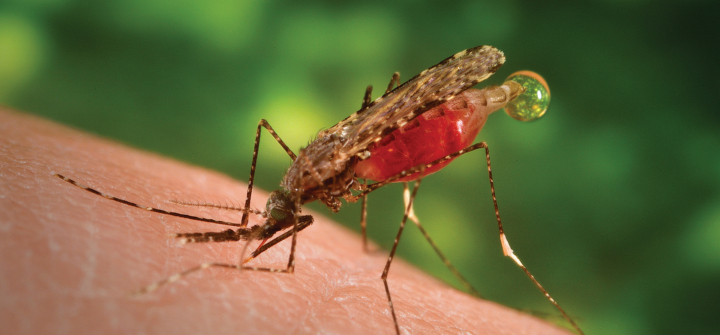
On August 20, 1897, Ronald Ross made his momentous discovery. The British medical officer in India, Ross found the malaria parasite in the “dapple-winged” mosquito. He marked the scientific breakthrough by penning these lines:
O million-murdering Death; I know this little thing; A myriad men will save.
Little thing, indeed.
As I wrote 5 years ago in GHN for World Mosquito Day, Sir Ronald’s discovery changed the world, breaking from the past “bad air” theories of malaria transmission and bringing us a new paradigm that has saved many millions over the decades.
Sadly, 5 years on, gains in global malaria control efforts have stalled. After significant progress in lives saved since the start of the millennium—made possible with increased funding to expand access to insecticide treated nets, indoor residual spraying, new diagnostics, and treatments—we are at a crossroads and no longer on track to meet our malaria elimination goals. There are several contributing reasons, including large populations displaced by conflict and severe weather, insecticide and drug resistance, and competing priorities with COVID-19 and Ebola. Part of the problem may also be us and our pre-pandemic systems.
Arundhati Roy published “The Pandemic Is a Portal” in the Financial Times on April 3, 2020, writing:
Historically, pandemics have forced humans to break with the past and imagine their world anew. This one is no different. It is a portal, a gateway between one world and the next. We can choose to walk through it, dragging the carcasses of our prejudice… our data banks and dead ideas. Or we can walk through lightly, with little luggage, ready to imagine another world. And ready to fight for it.
The accelerated pandemic response these past 2.5 years with new diagnostics, vaccines, and therapeutics, as well as the intense health care system response, carry lessons for global malaria efforts. The public sector commitment to work in partnership with the private sector to develop these technologies and expedite their review and deployment stands in stark contrast to the way we approach “the other emergency” of malaria.
We old malariologists often hold the commercial sector at arm’s length, as “vendors” rather than “partners,” competing in massive global tenders for the lowest possible unit cost. With insecticide treated nets, this cost drive to the bottom stifles innovation for durability and quality improvement, user acceptability, and incorporation of new chemistries to combat insecticide resistance.
The approval process for malaria products is still numbingly slow, years for innovations that may have already been approved for safety and efficacy by stringent regulatory authorities such as the US EPA. There are often demands for prohibitively expensive randomized control trials (RCTs) with epidemiological endpoints. While RCTs are the “gold standard” for therapeutics and vaccines, they may be inappropriate—and at times unethical—in context-specific environmentally driven processes like malaria transmission.
We can learn from the water, sanitation, and hygiene (WASH) sector, which is moving away from RCTs for WASH project evaluation into “transformative WASH,” beginning with human-centered design, stakeholder alignment, tailored evaluation designs, iterative program learning and scale-up, and the discovery not just what works, but why things work.
The other lesson of the past 2 years was our over-reliance on top-down “solution-implementation” rather than a bottom-up “problem-solving” capacity. As the attention of donors, ministries, and implementing partners was diverted to pandemic response, some, but not all, malaria programs foundered. Thankfully, there is interest by WHO to “Rethink Malaria” that includes capacity-building and decentralized decision-making at the subnational level. There are also initiatives for “new routes to market” for community access to lifesaving commodities that are not wholly dependent on government deployment systems.
The pandemic is a portal. I hope that on tomorrow’s “World Mosquito Day 2022” marking the day in 1897 we broke from the “bad air” theories, we heed Arundhati Roy, break from the past, learn the lessons from COVID-19, change our systems, and imagine a new path towards a malaria-free world.
Michael B. Macdonald, ScD, is a public health entomologist in Catonsville, Maryland.