From 'Condom Man' to Full-Service HIV Clinic: How One Team in Uganda Serves Key Populations
Mulira Aramanzani was working as a border guard in Busia, a town on Uganda’s Eastern border with Kenya, when he saw an opportunity.
The area was relatively private and remote, but a hub for some key populations who face the highest risk of contracting HIV. Yet there were no health services nearby for them.
Truck drivers, who are considered a key population, would stop, sometimes for days at a time before being cleared to cross the border. They’d pass the time at the Amalgamated Transport General Workers Union (ATGWU), a space where they could get a meal, play games, or watch TV, and spend the night. Some would engage with sex workers, another key population.
“I saw the challenges of those who were going through the border, and the truck drivers were asking for health services. I had the medical knowledge—I had my lab tech qualification. I said, we can start something here to support our key populations,” said Aramanzani, now 37 and ATGWU’s team leader and lab tech.
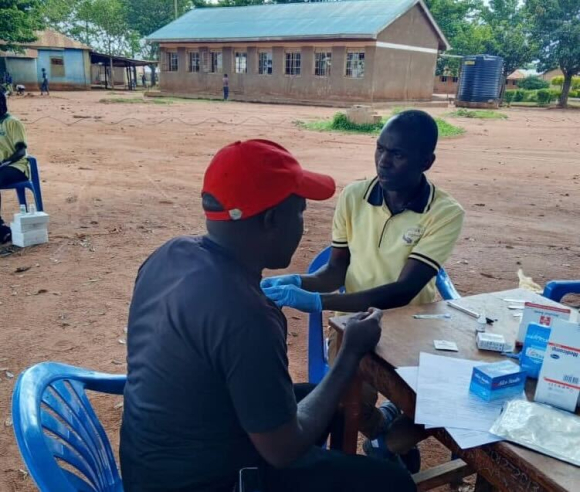
In 2010, with the help of a grant from FHI360, an organization that supports community-based efforts to tackle health challenges, he rented a room at ATGWU to serve key populations—mostly sex workers, men who have sex with men, people who use injectable drugs, and truck drivers—with basic offerings like condoms, lubricants, and information in a welcoming atmosphere that they wouldn’t get at government hospitals.
“These people don’t want to be seen in the government hospital because of the stigma,” he said. “They feel free here [at ATGWU]. At the government hospital people say, ‘Look at this MSM, look at this sex worker.’ They feel lonely at the government facilities. They are abused by health care workers.”
Initially, incorporating these services into a truck stop saw resistance from some members of surrounding community, including religious leaders and truck drivers who didn’t want their industry associated with HIV-related services. Aramanzani was ridiculed at first—even by the key populations he was serving. “They talked negatively. They called me ‘condom man.’ They were mocking me then—but it’s more of a nickname now.”
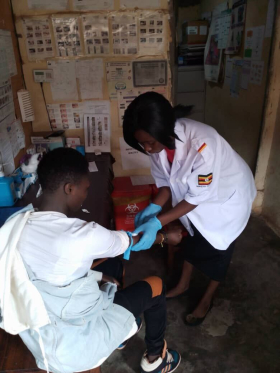
The border area was a hotspot for HIV transmission, and cases were ticking up, Aramanzani says. The drop-in center’s value and the demand it responded to were clear—but they needed to offer more.
By 2017, the project had expanded—largely funded by AHF Uganda Cares, one of Uganda’s largest providers of free HIV/AIDS treatment and care—to deliver clinical services including PrEP, antiretroviral treatment, and STI treatment. It built up a staff of counsellors, clinicians, lab techs, and crucially, peer leaders—members of key populations who engage their communities with the clinic and help maintain relationships with HIV-positive clients who are at risk of forgoing treatment.
Today, the drop-in center, known as ATGWU, provides ART for 315 individuals who return every six months to check their viral load and renew their medication. It provides PrEP for 1,600 clients and serves some three dozen daily walk-ins who come in for condoms, lubricants, HIV and STI testing—and somewhere to hang out and play pool or watch football.
An essential ingredient, says Aramanzani, is that the majority of ATGWU’s staff are part of the key populations they serve. “KPs are serving KPs.”
The theme of this year’s World AIDS Day —“Let Communities Lead”—highlights the essential role of community-driven services in the global fight against HIV/AIDS. It also acknowledges that the fight to end AIDS is being obstructed by dwindling funding to support these efforts, and harmful laws and policies that threaten people from populations at risk of contracting HIV.
In 2022, only about a tenth of the funding needed by 2025 for HIV prevention programs among people from key populations had been secured, according to UNAIDS. Last year, a total of $20.8 billion was available for HIV programs in low- and middle-income countries––well short of the $29.3 billion needed by 2025.
While the U.S. government—chiefly through PEPFAR—and the Global Fund supply almost 90% of international assistance for HIV, other donor contributions that make up the remaining funding have fallen by 61%, from $3 billion in 2010 to $1.2 billion in 2022.
Those cuts are being felt by ATGWU. “The demand is growing but the funding is shrinking,” Aramanzani says.

Aramanzani and other advocates fear that Uganda’s anti-homosexuality bill, signed in May promising sentences ranging from 10 years to the death penalty, has both endangered ATGWU’s clients and added to donor jitters.
In the months after the bill was signed, ATGWU’s budget was cut by 10%. They cut back on outreach services, reaching fewer people. For three months they had no condoms or lubricants to offer clients. They’re running low on PrEP and have been borrowing supplies from other facilities. In August, they cut two of their five counselors, and reduced pay for their peer leaders—who are paid with small stipends and meals—from $45 per month to $15.
Community engagement has also been essential in keeping ATGWU’s reputation intact after Uganda’s vaguely written anti-gay bill was used to justify reporting ATGWU clients to the police when they sought care. Aramanzani was lambasted for promoting homosexuality, which is banned in the law.

People said “Let them die. Don’t give them condoms—don’t give them those services,” said Aramanzani.
Four months later, in August, the Ministry of Health had produced guidelines clarifying that LGBTQ+ individuals had the right to seek health care irrespective of their lifestyle. Still, some community members, including religious leaders, had already used the law to justify reporting ATGWU’s clients to the police.
For months after the bill was signed, “MSM went into hiding,” and stopped turning up at ATGWU, says Aramanzani. Through outreach in community meetings and on talk radio, Busia district officials and ATGWU clarified the law. “We explained we are not recruiting, we are giving professional services,”Aramanzani says. While stigma remains a perennial challenge, they were able to quell some of the blowback.
“We explained to them, there could be somebody in your family that might be impacted, that might be in this group and you just don’t know it,” says Aramanzani. “They calmed down a bit.”
Join the 50,000+ subscribers in 170+ countries who rely on Global Health NOW summaries and exclusive articles for the latest public health news. Sign up for our free weekday newsletter, and please share the link with friends and colleagues.
All images courtesy of ATGWU





