Gender Equity Key to Providing Patients with Best Possible Surgical Care
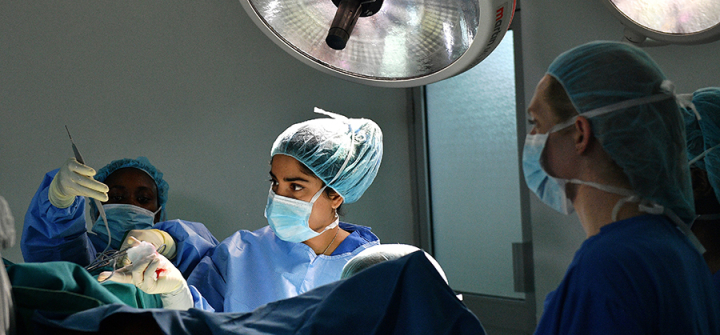
Sitting in a large auditorium, my eyes scanned across the 300 or so highly respected cardiothoracic surgeons who came from all over Japan. Many were dozing or fast asleep. All but 5 or 6 of the surgeons were men. The gender imbalance shocked me. It shouldn’t have.
Recently, Tokyo Medical University was found to be deliberately reducing test scores of female applicants to ensure that a maximum of 30% of the incoming class were women. This shameful practice had been going on since 2010 when the number of successful female applicants started rising sharply. Those involved “justified” their actions based on their presumption that more women drop out of clinical work after marriage or childbirth. Traditionally, Japan has been lagging in terms of female opportunities in the work sector and in particular the medical field, compared to other developed nations.
Institutional barriers faced by women in fields traditionally dominated by men are not reserved for Japan. In the US, medical school has only recently started welcoming more female students. In the 1970s, only 6% of medical students were female. Today, the number of female medical students has surpassed those of male students. Nevertheless, a wide range of factors continue to prevent women from going into surgery, including negative lifestyle perceptions, a lack of mentors and role models, and persistent and pervasive “old boys club” attitudes in most surgical disciplines. Today, only 19.2% of US surgeons are female, and the lack of representation in leadership is reflected by the fact that only 21 surgery departments are chaired by a female surgeon.
Gender disparities are also evident in surgeons’ pay. Female surgeons tend to earn 8% less on average compared to their male counterparts. Before the age of 35, female surgeons earn only 90% of what their male colleagues do. Shockingly, gaps increase with age; female surgeons over 35 earn only 82% of what male surgeons earn.
Despite this, women surgeons appear to perform equally well, if not better than their male peers when measured on medical knowledge, clinical judgement, technical and communication skills, and professionalism.
Finally, things are changing. In the US, successful female medical school applicants entering surgical residency have reached nearly 40%. The rise of organizations like the Association of Women Surgeons in the US and elsewhere is helping too. The Japanese Association of Women Surgeons (with the formidable acronym, JAWS) is working to change the social perception of women surgeons in Japan. “Now is the ideal opportunity to discuss not only how to maintain work-life balance regardless of gender, but also how to create more gender-equal environments,” says Kawase Kazumi, a breast surgeon, an associate professor of Surgery at the Jikei University School of Medicine in Tokyo, and JAWS founder. “Women surgeons cannot give up further efforts to show their talents and climb up the ladder.”
Embracing women surgeons is not only the right thing to do for our female colleagues; it is our duty and the intrinsic right of patients to receive the highest possible quality of care.
In 10 years, I hope an auditorium of cardiothoracic surgeons in Japan will demonstrate the presence and impact of female surgeons.
Perhaps that will help keep the audience awake.
Dominique Vervoort, MD, is a medical doctor from Belgium with previous clinical experience at Keio University Hospital in Tokyo, He currently works as a research associate at the Program in Global Surgery and Social Change at Harvard Medical School. Follow him on Twitter @DVervoort94.
Join the tens of thousands of subscribers in more than 100 countries who rely on Global Health NOW summaries and exclusive articles for the latest public health news. Sign up for our free weekday enewsletter, and please share the link with friends and colleagues: http://www.globalhealthnow.org/subscribe.html
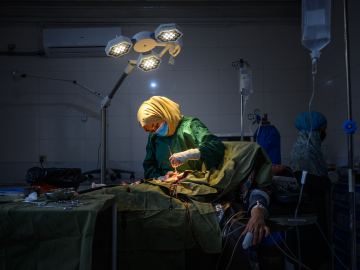
Surgeons are at work during restorative surgery on a survivor of female genital mutilation in Nairobi, Kenya on May 11, 2017. Image: Carl de Souza/AFP/Getty